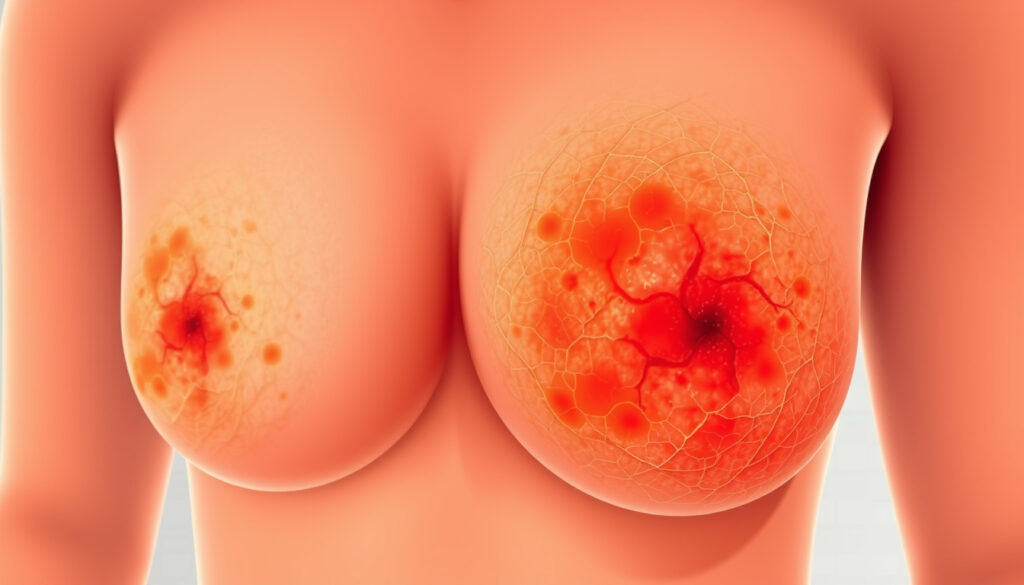
Pictures of Inflammatory Breast Cancer in Early Stages
A persistent patch of red or pink that doesn’t fade, a breast that feels heavier than usual, skin that looks like the peel of an orange—these can be easy to brush off as a rash or an allergic reaction. But for a small number of people, these changes signal something far more serious: inflammatory breast cancer (IBC), a rare and aggressive form of the disease that accounts for 1% to 5% of all breast cancers. Understanding what early-stage IBC looks like in pictures and in real life could be the difference between catching it at stage III and catching it earlier.
IBC accounts for up to 5% of all breast cancers American Cancer Society ·
Typically diagnosed at stage III or IV due to rapid progression National Cancer Institute ·
Median age at diagnosis is 57 years SEER data ·
One-year survival rate for localized IBC is 90% American Cancer Society
Quick snapshot
- Persistent pink or red area that does not fade (Breast Cancer Research Foundation)
- May start small then spread quickly (Breast Cancer Research Foundation)
- Does not respond to topical creams or antihistamines (Free Medical Journals)
- Breast feels heavy and enlarged (Massive Bio)
- Skin warm to the touch (Breast Cancer Research Foundation)
- Noticeable increase in bra cup size (Massive Bio)
- Dimpling like orange peel (peau d’orange) (Massive Bio)
- Thickened, ridged, or pitted skin (Breast Cancer Research Foundation)
- Welts or raised areas without clear borders (Breast Cancer Research Foundation)
- Nipple retraction or flattening (Breast Cancer Research Foundation)
- Discharge other than milk (Breast Cancer Research Foundation)
- Swollen lymph nodes under arm or above collarbone (National Cancer Institute)
Six key facts about IBC in context:
| Fact | Value |
|---|---|
| IBC percentage of all breast cancers | 1% to 5% (American Cancer Society) |
| Typical stage at diagnosis | Stage III or IV (National Cancer Institute) |
| 5-year survival rate (localized) | 90% (American Cancer Society) |
| Median age at diagnosis | 57 years (SEER data) |
| Median time from symptom to diagnosis | 3 to 6 months (National Cancer Institute) |
What does stage 1 inflammatory breast cancer look like?
Stage 1 IBC is rare, but when it does appear, the visual cues are distinct—and often surprising to patients who expect a lump. The hallmark is a persistent change in the breast’s appearance rather than a palpable mass.
Physical changes to the breast
- The affected breast may appear red, pink, or bruised over at least one-third of its surface (Breast Cancer Research Foundation)
- No discrete lump is typically present, making self-exams misleading (Massive Bio)
- Early IBC rashes may initially appear as an irritation of the skin or red bumps, or may look like bruising on one breast
Change in size, warmth, or color
- The breast may feel heavy, warm, or look inflamed (Breast Cancer Research Foundation)
- Rapid swelling can occur, with the breast increasing by one or more bra cup sizes in weeks
- In early-stage IBC, redness is localized or faint, while in advanced stage redness is diffuse and covers more than one-third of the breast (Free Medical Journals)
The absence of a lump means IBC is often missed during routine breast exams or mammograms. For patients, the first visible sign is usually a change in skin color or texture—not a bump they can feel. That’s why knowing what early-stage IBC looks like is a critical diagnostic tool.
The pattern: Stage 1 IBC is defined by visible skin changes without a lump—a presentation that mimics infection far more than typical breast cancer. The implication for patients: if redness and swelling persist beyond two weeks without improvement, imaging and biopsy are warranted even if mammogram is normal.
What does an early inflammatory breast cancer rash look like?
The rash of early IBC is one of its most recognizable features—and one of the most commonly mistaken. Unlike an allergic rash or contact dermatitis, IBC-related redness does not respond to creams or antihistamines.
Redness and rash appearance
- The rash often starts as a small area of pink or red that may resemble an insect bite or mild sunburn (Breast Cancer Research Foundation)
- It spreads quickly, covering more of the breast within days to weeks
- The skin may appear ridged or have small welts, and the breast may feel warm to the touch
Dimpling or peau d’orange texture
- Peau d’orange (orange peel texture) occurs when lymphatic vessels under the skin are blocked by cancer cells (Massive Bio)
- The skin looks bumpy, dimpled, and thickened, similar to the surface of an orange
- This texture change is not present in most benign rashes or infections
The IBC rash is often mistaken for mastitis, especially in younger women or those who are pregnant or breastfeeding. But mastitis typically improves with antibiotics within 48 hours. IBC does not. The diagnostic challenge: patients lose valuable weeks trying treatments that cannot work.
The catch: In patients with darker skin tones, early IBC redness can be under-recognized because the skin color change may appear as a subtle darkening or purplish hue rather than bright red (Free Medical Journals). The implication: women of color may experience longer delays in diagnosis.
How quickly do symptoms of inflammatory breast cancer appear?
Unlike other breast cancers that may develop over years, IBC symptoms progress rapidly—often within weeks to a few months. This aggressive timeline is both a warning sign and a diagnostic clue.
Weeks vs. months
- Symptoms can develop in weeks to months, not years (National Cancer Institute)
- Rapid swelling and redness are characteristic of IBC and distinguish it from other breast conditions
- The breast may change noticeably from one week to the next
Progression to advanced stage
- Most IBC cases are already stage III or stage IV by the time of diagnosis (National Cancer Institute)
- Cancer cells block lymphatic vessels in the skin, leading to sudden alterations in the breast’s appearance and feel (Massive Bio)
- Early diagnosis is critical because the cancer grows and spreads so quickly
“Inflammatory breast cancer grows and spreads rapidly, and prompt diagnosis and treatment are essential.”
— Mayo Clinic on IBC
What this means: The rapid progression of IBC creates a narrow window for intervention. For a patient who notices breast swelling or redness, waiting even two weeks to “see if it goes away” can mean the difference between localized disease and spread to lymph nodes.
What could be mistaken for inflammatory breast cancer?
IBC is frequently misdiagnosed as one of several benign conditions, leading to treatment delays. Knowing the key differences can help patients and clinicians avoid this pitfall.
Four conditions commonly confused with IBC, one key pattern: infection or allergy responds to treatment; IBC does not.
| Condition | Key features | How it differs from IBC |
|---|---|---|
| Mastitis (breast infection) | Redness, warmth, swelling; often during lactation | Responds to antibiotics within 48 hours; IBC does not (Free Medical Journals) |
| Cellulitis | Skin infection with warmth, redness, fever | Accompanied by fever and improves with antibiotics; IBC lacks fever (Free Medical Journals) |
| Allergic reaction | Itchy, patchy redness; no swelling | Lacks breast enlargement or peau d’orange texture; responds to antihistamines (Free Medical Journals) |
| Dermatitis or eczema | Dry, flaky, itchy skin | No deep tissue swelling; responds to moisturizers or steroids (Free Medical Journals) |
“IBC is frequently misdiagnosed as mastitis, especially in younger women or those who are pregnant or breastfeeding.”
— Massive Bio
The implication: The most reliable diagnostic test is treatment response. If antibiotics or antihistamines do not resolve breast symptoms within 48–72 hours, the next step should be imaging and possibly biopsy—even if no lump is felt.
What are all the symptoms of inflammatory breast cancer?
IBC symptoms can be remembered with the acronym “HARTS”—H: Hard, A: Appearance changes, R: Redness, T: Temperature, S: Swelling. But the full picture involves multiple systems.
Breast swelling and heaviness
- The affected breast may become noticeably larger than the other side
- Patients often report a feeling of heaviness or fullness (Breast Cancer Research Foundation)
- Swelling may be accompanied by a feeling of warmth
Skin redness, dimpling, or ridges
- Redness affects at least one-third of the breast surface
- Skin may appear dimpled like an orange peel (peau d’orange)
- Ridges or welts may appear, and the skin can feel thickened (Massive Bio)
Nipple retraction or discharge
- Nipple inversion or flattening can occur (Breast Cancer Research Foundation)
- Discharge other than breast milk may be present
- Lymph node swelling under the arm or above the collarbone is common
IBC symptoms affect the breast in a “block” pattern—covering at least one-third of the breast surface—rather than as a localized spot. If you see redness, swelling, and texture change that involve most of one breast and persist for more than two weeks, do not wait for a lump to appear. Request imaging and a referral to a breast specialist.
Why this matters: IBC’s symptom constellation—redness, swelling, warmth, skin changes, and nipple retraction—mimics infection so closely that 50% of cases are initially misdiagnosed. For patients, the key signal is combination: redness plus swelling plus texture change without fever or response to antibiotics.
What age is most common for inflammatory breast cancer?
IBC affects women slightly younger than those with other breast cancers, and the racial disparities in diagnosis age are striking.
Age distribution
- Median age at diagnosis is 57 years (SEER data)
- IBC occurs at a slightly younger age compared to other breast cancers, which have a median age of 62
- Black women present at younger ages on average than White women (National Cancer Institute)
Risk factors
- Obesity is a known risk factor for IBC
- Younger age at first childbirth may also increase risk
- Family history plays a smaller role than in other breast cancers, though the exact cause is unknown
“The exact cause of inflammatory breast cancer is unknown, but it is not linked to the same genetic mutations as other breast cancers.”
The pattern: The younger median age and higher incidence in Black women mean that IBC should remain on the differential for any woman in her 40s or 50s presenting with unilateral breast swelling and redness—especially if she is not breastfeeding.
Timeline
IBC’s history in medical understanding spans two centuries, with key milestones in recognition and treatment.
- 1824 — First medical description of inflammatory breast cancer by Sir Charles Bell (PubMed/National Library of Medicine)
- 1970s-1980s — IBC recognized as distinct clinical entity; multi-modality treatment introduced (National Cancer Institute)
- 2008 — World IBC Awareness Week established
- Ongoing — Trials focus on targeted therapies, immunotherapies
The implication: Despite being described nearly 200 years ago, IBC remains under-recognized today. The lag between first symptom and diagnosis—typically 3 to 6 months—has not shortened significantly in the past two decades, pointing to persistent gaps in awareness.
Confirmed facts vs. what remains unclear
Confirmed facts
- IBC is a rare, aggressive breast cancer that accounts for 1% to 5% of all breast cancers (American Cancer Society)
- Symptoms appear quickly (weeks to months) (National Cancer Institute)
- Imaging and biopsy are required for diagnosis (Breast Cancer Research Foundation)
- Most IBC patients do not have a lump
- Antibiotics do not improve IBC symptoms
What’s unclear
- Exact cause is unknown (National Cancer Institute)
- Why IBC affects Black women at younger ages is still under study
- The molecular mechanism behind the rapid spread is not fully understood
- Why some cases respond to treatment while others do not is an open question
The implication: Understanding what is confirmed and what remains uncertain helps patients and clinicians navigate diagnosis and treatment decisions with realistic expectations.
healthcentral.com, theibcnetwork.org, medicalnewstoday.com, mdanderson.org
For a clearer understanding of early-stage inflammatory breast cancer, a visual guide across skin tones shows how symptoms appear on different skin tones.
Frequently asked questions
How is inflammatory breast cancer diagnosed?
Diagnosis typically involves a combination of clinical breast exam, mammogram or ultrasound, MRI, and biopsy of the breast skin or tissue. A pathologist looks for cancer cells blocking the lymphatic vessels in the skin (Breast Cancer Research Foundation).
Can inflammatory breast cancer be seen on mammogram?
Mammograms can show skin thickening, trabecular thickening, and breast enlargement, but IBC often does not form a distinct mass that appears on standard mammography. MRI or ultrasound may be more sensitive (National Cancer Institute).
What does inflammatory breast cancer feel like?
Patients often describe a feeling of heaviness, fullness, or firmness in the affected breast. The breast may feel warm to the touch, and the skin may feel thickened or tight. Some report a burning sensation or tenderness (Breast Cancer Research Foundation).
Is inflammatory breast cancer hereditary?
IBC is not strongly linked to the BRCA1 or BRCA2 gene mutations associated with other types of breast cancer. Most cases are sporadic, meaning they occur without a known family history (National Cancer Institute).
Can men get inflammatory breast cancer?
Yes, men can develop IBC, although it is very rare. Male breast cancer accounts for less than 1% of all breast cancers, and IBC in men is even less common (National Cancer Institute).
What is the treatment for inflammatory breast cancer?
Treatment typically involves neoadjuvant chemotherapy first (before surgery), followed by mastectomy and radiation therapy. Targeted therapies and hormone therapy may be used if the cancer expresses appropriate receptors. Clinical trials for immunotherapies are ongoing (Mayo Clinic).
How long can you live with inflammatory breast cancer?
Survival depends on stage at diagnosis and treatment response. The 5-year survival rate for localized IBC is about 90%, but drops to around 50% if the cancer has spread to regional lymph nodes, and lower still if distant metastasis is present (American Cancer Society).
Can inflammatory breast cancer be cured?
IBC can be cured if caught early and treated aggressively. Complete remission after neoadjuvant chemotherapy followed by mastectomy offers the best prognosis. However, because IBC is often diagnosed at an advanced stage, cure rates are lower than for other breast cancers (National Cancer Institute).
For anyone who notices persistent breast redness, swelling, or skin changes that do not improve with antibiotics or antihistamines, the choice is clear: see a healthcare provider for imaging and evaluation without waiting for a lump to develop. The difference between early-stage IBC and advanced IBC can be measured in weeks—and early action is the single best predictor of a good outcome.
Related reading